Understanding the role of research


Years

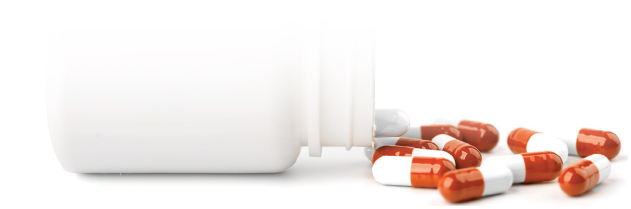 12 years
12 years
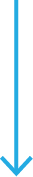
In 2019, our national peer-reviewed Research Program awarded $2.1 million to 20 researchers across the country working on projects to find the cause and the cure, as well as effective treatments, for Alzheimer's disease and other dementias.
Our Program is one of the few in Canada that focuses solely on dementia research. Fifty per cent of our funds are directly invested in producing advances in science, from improving diagnosis to finding cures, while 50 per cent go towards enhancing practices and care in order to ensure Canadians affected by dementia live as best possible in their homes and their communities.
During the 2018-19 period, we celebrated the completion of Phase I of our partnership with the Canadian Consortium for Neuro-degeneration in Aging (CCNA). To date, we have invested close to $3 million in CCNA-led research.
We are grateful to donors for their generous support and to the fundraising efforts of our provincial Alzheimer Society partners.
The Alzheimer Society of Canada is a founding partner and the lead funder of the CCNA through the Alzheimer Society Research Program. Established in 2014, the Canadian Consortium for Neurodegeneration in Aging is a nationwide collaborative platform that includes more than 350 clinicians and researchers who are investigating Alzheimer's disease and other age-related neurodegenerative diseases, with a focus on prevention, treatment and quality of life.
During Phase I, we supported these important areas of the CCNA's work to help accelerate the development of new dementia treatments and improve care:
Dr. Claude Vincent is passionate about improving care and support for people living with dementia. She is leading the first Canadian study that looks at whether people with dementia and their caregivers can benefit from the full-time support of a dog. Dr. Vincent's research team is assessing the impact of both regular companion dogs and certified assistance dogs—known as "Dementia Dogs." These dogs are trained to provide cues and companionship and can help encourage physical activity, improve wayfinding, and enhance well-being and connection. Previous studies have shown that support animals can help improve quality of life for people living with other disabilities, and now Dr. Vincent and her team hope to demonstrate this same positive impact for people living with dementia. The results of her study will help families living with dementia understand the potential benefits of having a companion animal in their home, while also informing the development of new in-home support programs.
"Funding options are very limited for this type of research, but it is so important. The Alzheimer Society Research Program may be the best way to develop new approaches to improve the quality of life of people living with dementia and their caregivers." —Dr. Claude Vincent

Dr. Gordon Francis wants to get to the root of what causes dementia. That's why he is investigating the connection between dementia and cerebral amyloid angiopathy (CAA)—a neurological condition where a protein called beta-amyloid builds up on the walls of the arteries in the brain. CAA increases a person's risk of both stroke and dementia. Dr. Francis and his team believe that when arteries in the brain are damaged by "lifestyle" risk factors, including high blood pressure, smoking, diabetes and high cholesterol—as well as through the normal aging process—their ability to clear the sticky beta-amyloid proteins is reduced.
Proving this connection would mean that reducing lifestyle-related risk factors could be a form of early treatment to prevent or reduce the development of CAA and the dementias that can result from it.
DID YOU KNOW? Having a stroke more than doubles your risk of developing dementia.

Dr. Fernanda De Felice wants to find ways to protect the brain from the devastating effects of Alzheimer's disease. Dr. De Felice is studying a protein called irisin, sometimes referred to as "the exercise hormone" because it is released by muscles during physical activity. She believes that irisin could help preserve memory for people living with Alzheimer's disease and other dementias. In previous research, her team found that people with Alzheimer's have less irisin in the brain—and when that irisin is depleted, new memories aren't formed. If the decrease of irisin in the brain can be counteracted through medication or exercise, this may be a way to keep brain cells and synapses healthy and lead to new treatments to combat dementia.
DID YOU KNOW? Regular physical exercise can reduce your risk of developing Alzheimer’s disease by up to 50 per cent. Exercise can also slow further deterioration in people who have already started to develop cognitive problems.

Dr. Andrea Leblanc has received support from the Alzheimer Society Research Program since 1995. Early in her research, Leblanc suspected that amyloid deposits—which are found in abnormally large amounts in the brains of those with Alzheimer’s disease—were a consequence of the disease rather than the cause, as many others hypothesized.
Over 20 years later, Leblanc’s search for alternative causes of neurodegeneration has identified a link between caspase enzymes in the brain that cause inflammation, and the breakdown and death of neurons—a hallmark of Alzheimer’s disease and other dementias. Even more promising: Dr. Leblanc’s lab has had success using an existing drug (originally developed to treat inflammatory diseases) to reverse cognitive impairment and inflammation and inhibit amyloid deposits in mice. The next step is to test the drug in humans.
“Independent of whether one believes amyloid is the cause, neuronal degeneration, defined by the inability of neurons to perform normally due to their altered structure, needs to be stopped and that pathology reversed,” says Dr. Leblanc, who hopes to see the drug move into the clinical trial phase in the near future. Because the drug has already been proven safe for humans, this could happen more quickly than with a brand-new drug.
DID YOU KNOW? Several students in Dr. Leblanc’s research team are also currently funded by the Alzheimer Society Research Program and are investigating the role of caspases in Alzheimer’s disease.



Dear Alzheimer Society:
I’m an 18-year-old girl from Ottawa, Ontario. I have sent you this cheque for $3,500 that I would like to go toward Alzheimer’s research. I have also attached a list of the people who contributed to this donation.
In January of this year I lost one of the most important people in my life. His name was Eugene and he was my grandfather. He was diagnosed with Alzheimer’s disease 12 years ago. He was only 65 at the time. I can faintly remember the early symptoms, the forgetfulness and slight confusion, but he was still a happy and healthy man. Things started to get more emotionally difficult when he began to forget each of us … I can never truly tell you the pain I felt when he looked at me with that blank stare. He didn’t know me anymore; it was as if I was erased.
The last two years of his life were the toughest. He lost his ability to dress and feed himself, he became easily agitated, and he barely spoke a word to anyone … I understand that I’m not the only person in this world who had to go through this, and we are only one family out of millions who have or are currently going through the same thing.
I will always hate Alzheimer’s, from the day my grandfather got it to the day he died and until the day someone finds the cure. I hope that this donation will help get us to that point soon because unfortunately it wasn’t soon enough for him.
Adrianna